An interview with Yvonne Drasovean, RT Respiratory Therapy Program
When many people hear the word ventilator, they think of medical emergencies. COVID-19 brought ventilators into public conversation in a big way, often associating them with crisis. However mechanical ventilators are used in far more situations than many realize, from supporting premature babies and surgical patients to helping people manage chronic respiratory or neuromuscular conditions. Understanding what a ventilator is, how it works and who may need one offers a clearer picture of modern healthcare and the critical role respiratory professionals play.
What is a ventilator?
A ventilator, also called a mechanical ventilator, is a medical device that helps a person breathe when they cannot do so effectively on their own.
Sometimes, it provides breathing support. Other times, it temporarily takes over the full breathing process. A ventilator helps move oxygen into the lungs and removes carbon dioxide from the body, supporting essential functions when illness, injury or medical treatment affects normal breathing.
“A ventilator is sometimes referred to as an artificial lung, although it is not a lung itself. However, it performs a similar role by moving air to help deliver oxygen and remove carbon dioxide from the body.”
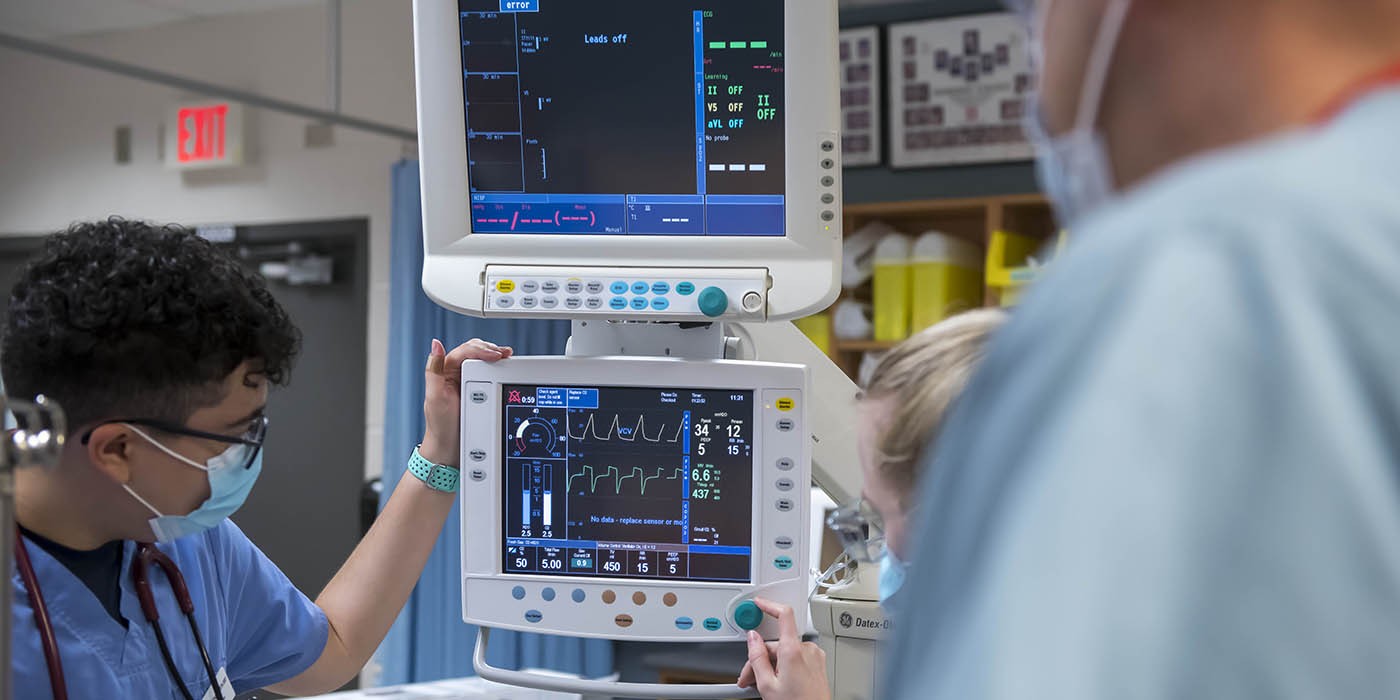
How does a ventilator work?
At its core, a ventilator uses controlled air pressure to move air in and out of the lungs. That sounds simple, but behind that process is a careful balance of physics, anatomy and physiology. Respiratory professionals must understand airflow, pressure, lung function, oxygen delivery and how the body responds to changes in breathing support.
Depending on a patient’s needs, a ventilator may connect through:
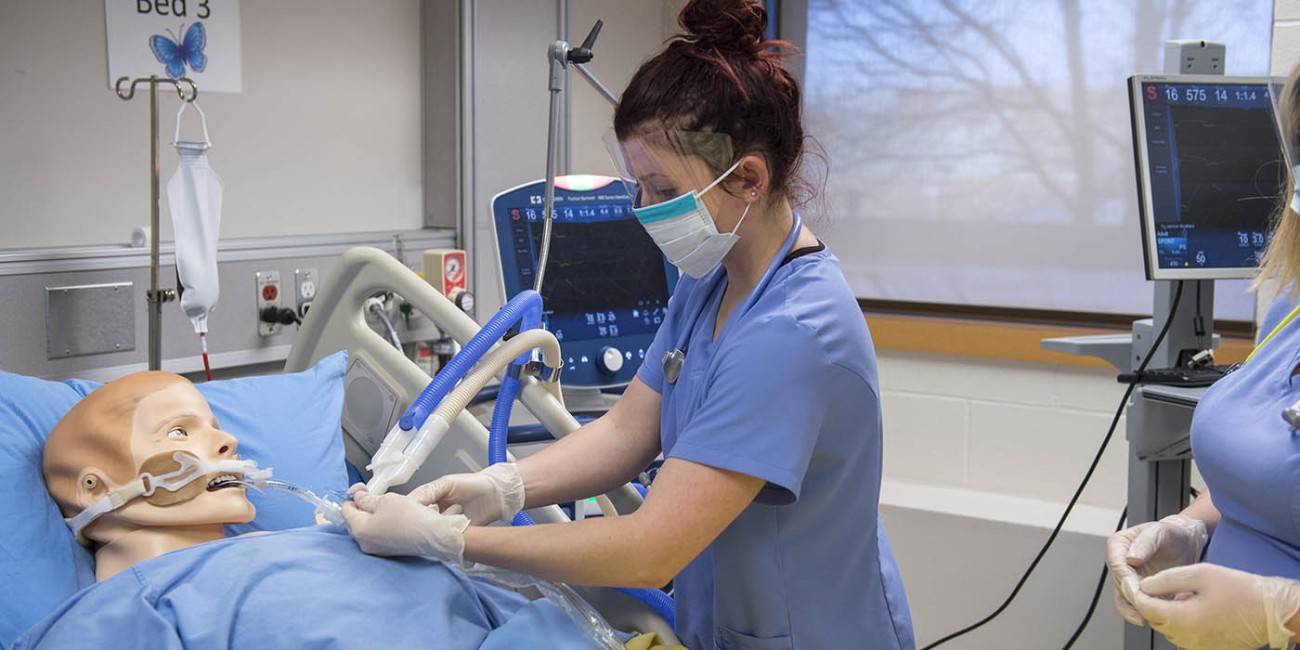
Endotracheal tube
A breathing tube inserted through the mouth, often used in intensive care units or surgery.
Non-invasive ventilation
Masks such as CPAP or BiPAP, commonly used for sleep apnea or milder respiratory distress.
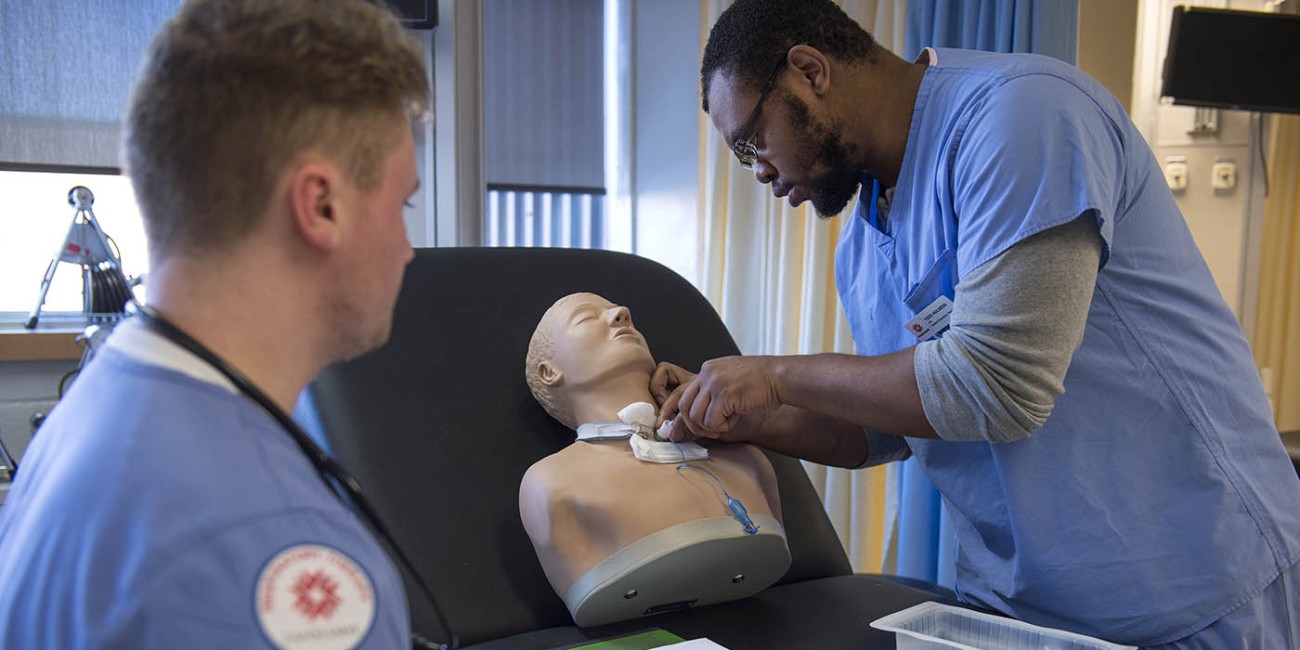
Tracheostomy
A surgical opening in the neck that provides long-term or emergency airway access.
Each method serves a different purpose, and each requires skilled clinical judgment.
Who may need a ventilator?
Ventilators support people across all stages of life.
From newborns to seniors, ventilation can become essential when breathing is compromised by illness, surgery or muscle weakness.
Severe pneumonia or COVID-19
Serious infections can inflame the lungs and reduce oxygen transfer, making breathing difficult or impossible without support.
Chronic obstructive pulmonary disease (COPD)
In advanced COPD or severe flare-ups, weakened lungs may struggle to move enough air.
Acute respiratory distress syndrome (ARDS)
ARDS can rapidly damage the lungs through inflammation and fluid buildup, requiring highly controlled ventilation.
Neuromuscular conditions
Diseases such as ALS, spinal cord injuries or Myasthenia Gravis may weaken the muscles needed for breathing, even if the lungs themselves remain functional.
Premature birth
Some premature infants are born before their lungs are fully developed and may need temporary respiratory support.
Surgery requiring general anesthesia
Even healthy patients often need ventilation during surgery because anesthesia can temporarily stop independent breathing.
“Your breathing muscles are paralyzed too. That’s why we use ventilators in every operating room.”
Can you live with a ventilator at home?
Modern portable ventilators allow some individuals with chronic conditions to live at home, attend school, work and travel with proper support systems. This is especially important for people with progressive neuromuscular diseases or long-term respiratory conditions. Home ventilation often involves not just the patient, but also family members and caregivers who are trained to monitor equipment, respond to alarms and recognize when medical support is needed. Respiratory Therapists may also provide ongoing in-home monitoring and education.
Are there risks to mechanical ventilation?
Like any medical intervention, ventilation requires precision. One major risk is barotrauma, which is lung injury caused by excessive air pressure. As lungs are delicate, ventilator settings must be carefully tailored to each patient’s condition.
This isn’t a one-size-fits-all machine.
Safe ventilation depends on trained professionals who understand both the technology and the patient behind it.
Why respiratory therapists matter
Ventilators are advanced machines, but technology alone isn’t enough. Respiratory Therapists are trained to assess patients, manage airways, monitor ventilator settings, troubleshoot emergencies and independently operate ventilators in a range of healthcare environments.. From operating rooms and intensive care units to neonatal care and home support, RTs play a critical role in ensuring breathing support is safe, effective and responsive.
“Ventilators have become more advanced, more sensitive and more adaptive to patients’ needs but they still require skilled hands and good clinical judgment.”
More than a crisis tool
Ventilators are often associated with worst-case scenarios. The reality is broader. They support life in countless healthcare settings every day, helping patients recover from surgery, manage chronic illness, survive severe respiratory disease and navigate complex medical conditions.
Understanding what a ventilator is means understanding more than a machine. It means recognizing the science, care and expertise required to support something we often take for granted: every breath.
This article was developed by Swapthika Nallavelli, Marketing Management student. Brought to you in collaboration with Village Creative, an experiential learning opportunity at Fanshawe College.
For any media inquiries, please reach out to mediainquiries@fanshawec.ca
Recent News
-
May 21, 2026
Fanshawe has strong showing at 2026 Skills Ontario Competition
Read StoryEighteen students representing Fanshawe’s Faculty of Science, Trades, Technology and Design and the... -
May 20, 2026
PWHL expansion marks major milestone for women’s hockey
Read Full AdvisoryThe Professional Women’s Hockey League (PWHL) has announced a significant expansion, adding teams in... -
May 14, 2026
Measles Symptoms, Complications & Prevention: Respiratory Risks Explained
Read OpinionLearn the symptoms of measles, its respiratory complications like pneumonia, and how vaccination and public health strategies prevent outbreaks.
Recent News
-
May 8, 2025
Construction Delays
Read StoryDue to ongoing construction in the area, there may be delays in reaching our clinic. We kindly ask... -
April 15, 2025
New Spring Schedule
Read StoryWe’re excited to announce that the spring schedule is now available on our website as we transition... -
December 16, 2024
2025 Pricing Adjustment
Read StoryEffective January 1st, our fees will increase to $30 per treatment. We understand that this is a...