An interview with Greg Donde, RRT, MSc, FCSRT, faculty Respiratory Therapy
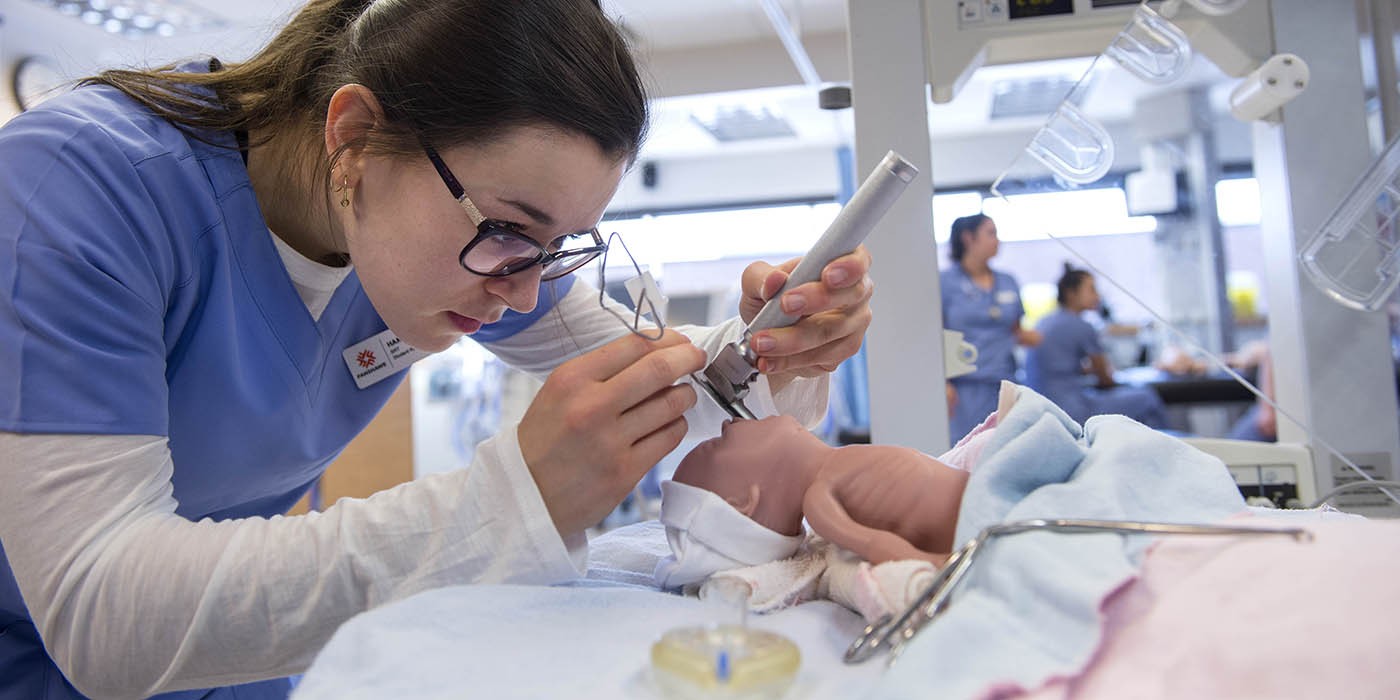
When a premature baby is born, one of the first and most urgent concerns may be breathing. This is where a respiratory therapist plays a critical role. For babies born prematurely or with respiratory risk factors, respiratory therapists are often among the first healthcare professionals to assess breathing, provide immediate support and guide care from delivery through treatment in the neonatal intensive care unit (NICU). For many families, this work happens behind the scenes, but in neonatal care, those first moments can be essential.
What does a respiratory therapist do in the delivery room?
Respiratory therapists are often part of the delivery or resuscitation team when a baby is born with known risk factors. This may include extremely premature births or situations where breathing complications are anticipated.
“Typically a respiratory therapist will attend any delivery of a baby who has risk factors. If it’s an extremely premature birth, there may be two RTs, two nurses, a medical fellow, a nurse practitioner, and a physician present.”
In these moments, respiratory therapists may:
- Assess breathing immediately after birth
- Provide oxygen
- Initiate positive pressure ventilation
- Perform intubation if needed
Their role often begins immediately after delivery.
How respiratory therapists support babies in the NICU
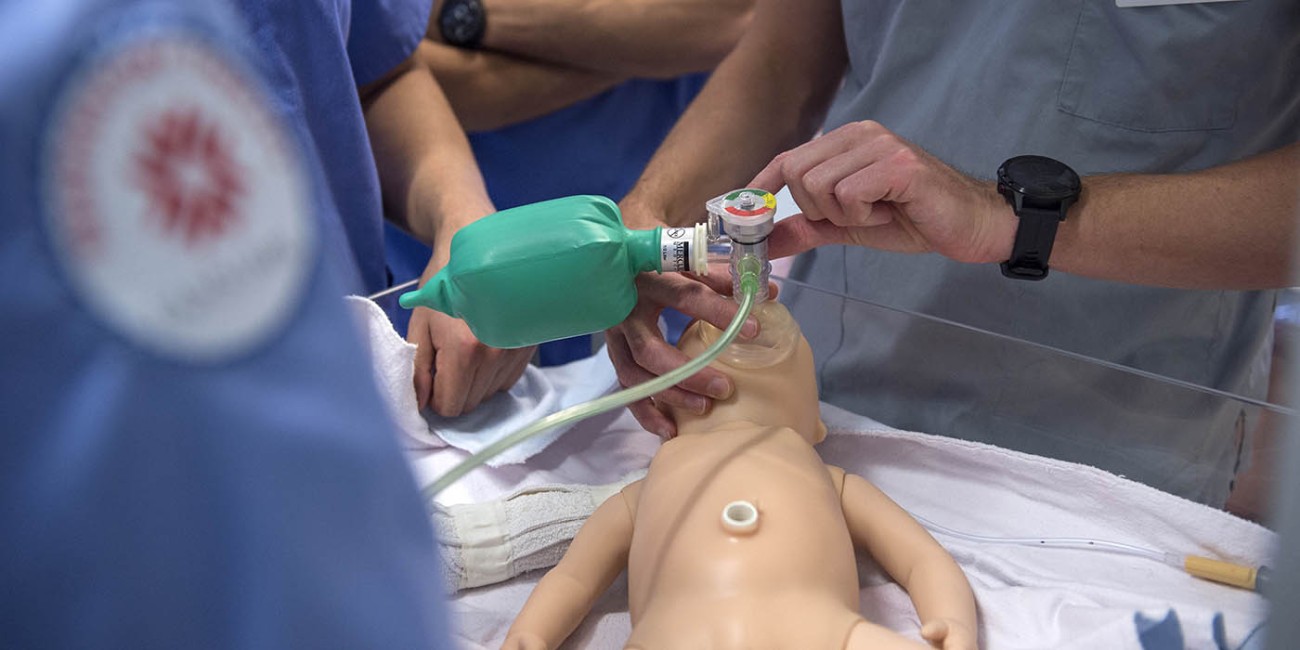
Premature babies may have underdeveloped lungs, making respiratory support especially important. Respiratory therapists in NICU settings help determine whether a newborn may benefit from non-invasive support such as CPAP or require more advanced respiratory support through mechanical ventilation.
This includes:
CPAP
A non-invasive approach used to support breathing.
Mechanical ventilation
A more advanced form of support when breathing assistance is more intensive.
Respiratory therapists apply respiratory interfaces, monitor effectiveness and make real-time adjustments to oxygen and pressure levels.
What role do respiratory therapists play in surfactant delivery?
For some premature babies, surfactant may be administered to support lung function. Respiratory therapists may deliver surfactant directly into the lungs through an endotracheal tube or other minimally invasive approaches.
“Sometimes we intubate to give surfactant, then extubate quickly to avoid lung trauma.”
This reflects the balance between providing effective support and minimizing potential lung injury.
What is NICU ventilation?
NICU ventilation involves specialized respiratory support for newborns who need help breathing, often using carefully controlled mechanical ventilators designed for neonatal care. Respiratory therapists are responsible for setting up, monitoring and adjusting ventilators based on each baby’s needs.
This may include advanced systems such as:
- High Frequency Oscillatory Ventilation (HFOV)
- High Frequency Jet Ventilation (HFJV)
These approaches use rapid, gentle breaths to support gas exchange while reducing the risk of long-term lung damage. Respiratory therapists closely monitor blood gases, oxygen saturation, respiratory patterns and ventilator performance. This requires ongoing assessment and adjustment.
Why clinical judgment matters
Respiratory therapists in NICU environments work as part of a larger care team. They collaborate with neonatologists, nurses and other healthcare professionals to adapt care based on each infant’s condition.
Their clinical judgment can influence:
- Immediate interventions
- Ventilation strategies
- Monitoring decisions
- Long-term care planning
In neonatal care, technical skill and collaboration go hand in hand.
How respiratory therapists are trained for NICU care
All respiratory therapists in Canada receive neonatal education as part of their training. This includes NICU exposure and hands-on experience with newborn respiratory care.
“Every RT student spends time in a NICU during training and gets hands-on experience with real deliveries. You could be working in a small-town hospital and find yourself responsible for a newborn in distress—it’s part of the job.”
This prepares respiratory therapists for a range of healthcare environments.
More than breathing support
So, what does a respiratory therapist do? In neonatal care, they assess, stabilize and support some of the most vulnerable patients from their very first breaths. From delivery room care to NICU ventilation and long-term support, respiratory therapists play a vital role in helping premature babies navigate complex respiratory challenges.
For some newborns, breathing support begins immediately and respiratory therapists are often there from the start.
Article created by Vansh Paul,, Marketing Management student. Brought to you in collaboration with Village Creative, an experiential learning opportunity at Fanshawe College.